Glute medius targeting training exercise.
/Subscriber video can be found at https://www.patreon.com/thegaitguys
Subscriber video can be found at https://www.patreon.com/thegaitguys


We think about the gluteus medius often, mostly, during stance phases of locomotion. But, do not forget about the absolutely necessary function of the gluteus medius on the swing limb. Foot placement of that swing leg is in part dictated by how well the pendulum leg receives gluteus medius control to abduct the leg. When it fails to abduct adequately, a more adducted/medial foot placement occurs (think deeply about our long posts and podcast rants on the cross over gait, the narrow based walking and running gait style).
An agreeable balance between the abductors and adductors affords a more pure forward saggital pendulum of the hinging leg. When imbalanced, from insufficient gmedius and the rest of the abductory team, the foot and leg can target a more medial pendulum swing and thus a more medial foot target placement. Thus, the gluteus medius is important in both the stance and swing phases of gait. Failure to develop the skill, endurance and strength of the gluteus medius and related complex of muscles during stance AND swing phases will often result in frontal plane pelvis drift on the stance limb, and adduction targeting of the foot (narrow step width). What is this called ? We call it the Cross Over gait and we have written oodles of articles about this gait phenomenon, more than anyone else. It is real, it has economical advantages and similar liabilities. Want to learn more, type it into the SEARCH box on our website-blog. Many people thinkn this is a normal gait, how we should all walk and run. And they are wrong, in part. Like most things, it has a place, but not a permanent place. We think like most things in this world, there is a benefit and a drawback to things, and it is how you use it, as long as you read the instructions. Sadly, we were never given a "users manual" when we were born, so we all did what felt natural and safe. It doesn't mean it was right.
-Dr. Shawn Allen
For our Patreon patrons:
read and digest this post again before i film a video of a critical exercise we use to train the gluteus medius in BOTH PHASES ! All to often people just train the glute medius in the stance phase, and that is critical, but the swing phase is just as critical ! And this exercise i will film and post up on Patreon in the next 24 hours or so will help with this swing phase, but stance phase too. Be sure, when you study the video, that you do not get bogged down in what the exercise looks like. That is the easy part. For you to train yourself and your client, there MUST be a deep understanding of the specifics of the exercise. You have likely seen versions of this exercise other places, but it is the how and the why, and not getting sloppy with it, that is the key factor.
Photo: this came in an old box of Altra shoes, a brochure. We love Altras, they aren't for everyone, but if you are looking for a lower heel drop shoes with a wide toe box, try out a pair !
Some sources say foot strike pattern does not matter. We disagree.
Look at this gal who midfoot/forefoot strikes. She also has a forefoot supinatus, a plastic condition where the forefoot is inverted with respect to the rearfoot. Take that combination and put it in a shoe with a forefoot flare and what do you get? Can you say AMPLIFICATION?
We’re not saying this is a bad shoe or even the wrong shoe. But, if she is going to run in this shoe, we will need to help her gain more ROM in her forefoot ( and some pelvic and hip stability) dodge doesn’t have to crash into eversion on each landing.
Help your patients with shoe selection. Something with less of a lateral flare in the forefoot would certainly make her life easier.
Need to know more? Consider taking our National Shoe Fit Program: link here:
Dr Ivo Waerlop, one of The Gait Guys
#badshoes #forefootflare #thegaitguys #forefootsupinatus #lateralflare #inversion
So a patient presents with forefoot pain, worse in the am upon awakening, with 1st weight bearing that would improve somewhat during the day, but would again get worse toward the end of the day and with increased activity. It began insidiously a few months ago (like so many problems do) and is getting progressively worse. Rest, ice and ibuprofen can offer some relief. You may see a dropped metatarsal head and puffiness and prominence in that area on the plantar surface of the foot, maybe not. Maybe you do a diagnostic ultrasound and see a lesion of the plantar plate as well? How did it get there?

image courtesy of Tom Michaud: with permission
Lets look at the anatomy of the short flexors of the foot, as well as some biomechanics of the foot, ankle and hip.
The flexor digitorum brevis (FDB) is innervated by the medial plantar nerve and arises from the medial aspect of the calcaneal tuberosity, the plantar aponeurosis (ie: plantar fascia) and the areas bewteen the plantar muscles. It travels distally, splitting at the metatarsal phalangeal articulation (this allows the long flexors to travel forward and insert on the distal phalanges); the ends come together to divide yet another time and each of the 2 portions of that tendon insert onto the middle of the middle phalanyx (1)
As a result, in conjunction with the lumbricals, the FDB is a flexor of the metatarsophalangeal and proximal interphalangeal joints. In addition, it moves the axis of rotation of the metatasophalangeal joints dorsally, to counter act the function of the long flexors, which, when tight or overactive, have a tendency to drive this articulation anteriorly .Do you see any subtle extension of the metatarsophalangeal joint and flexion of the proximal interphalangeal joints on your exam?
We know that the FDB contracts faster than the other intrinsic muscles (2), playing a role in postural stability (3) and that the flexors temporally should contract earlier than the extensors (4), assumedly to move this joint axis posteriorly and allow proper joint centration. When this DOES NOT occur, the metatarsal heads are driven into the ground, causing irritation and pain.
If there is also a loss of ankle rocker this problem is made (much) worse. Why? Because, with the loss of one rocker, another must make up for the loss: ankle rocker decreases, forefoot rocker has to increase; this equals increased metatarsal head pressure.
If you have been with us for any length of time, you know that ankle rocker and hip extension are intimately related, as one should equal the other, something we call “The “Z” angle”, that you have probably (hopefully?) read about here before.
So what is the fix? Getting the FDB back on line for one.
How about the toe waving exercise?
How about the lift spread reach exercise?
How about retraining ankle rocker and improving hip extension?
How about an orthotic with a metatarsal pad in the short term?
How about some inflammation reducing modalities, like acupuncture, ice laser and pulsed ultrasound.
Maybe some herbal or enzymatic anti inflammatories?
Dr Ivo Waerlop, one of The Gait Guys.
#gait #footpain #metatarsalgia #metatarsalpain #anklerocker #hipextension #thegaitguys
1. http://en.wikipedia.org/wiki/Flexor_digitorum_brevis_muscle
2. Tosovic D1, Ghebremedhin E, Glen C, Gorelick M, Mark Brown J.The architecture and contraction time of intrinsic foot muscles.J Electromyogr Kinesiol. 2012 Dec;22(6):930-8. doi: 10.1016/j.jelekin.2012.05.002. Epub 2012 Jun 27
3.Okai LA1, Kohn AF. Quantifying the Contributions of a Flexor Digitorum Brevis Muscle on Postural Stability.Motor Control. 2014 Jul 15. [Epub ahead of print]
4. Zelik KE1, La Scaleia V, Ivanenko YP, Lacquaniti F.Coordination of intrinsic and extrinsic foot muscles during walking.Eur J Appl Physiol. 2014 Nov 25. [Epub ahead of print]

The stuff we get/see.
Hallux amputation.
What would you expect to present in this case ?
We will dive into this one next week, but here are some cursory things to consider:
It is the right foot.
-Without the hallux, we cannot wind up the windlass and shorten the distance between the first metatarsal and heel, thus the arch will splay (more permanently over time we suspect) and we cannot optimize the arch height.
This will promote more internal spin on that limb because of more midfoot pronation and poor medial foot tripod stabilization.
- more internal limb spin means more internal hip spin, and more demand (which might not be met at the glute level) and thus loads that are supposed to be buffered with hip stabilization, will be transferred into the low back, and or into the medial knee. Look for more quad protective tone if they cannot get it from the glutes. Troubles arise when we try to control the hip from quadriceps strategies, it is poorly postured to do so, but people do it everyday, *hint: most cyclists and distance runners to a large degree)
- anterior pelvis posturing on the right, perhaps challenging durability of the lower abdominals, hence suspect QL increased protective tone, possible low back tightness or pain depending on duration of activities
- there is so much more, we are just wetting your appetite here on this one.
see you next week on this one gang !
Ivo and i are in the studio for another podcast this afternoon, hope you got to #137 this week ! lots more goodies to come !
cheers, shawn and ivo
Photo permission by patient


Why would you name a muscle after its supposed function when its function is actually something totally different? Probably due to what made sense from how it looked, not by how it acted. Of course, we are talking about the abductor hallucis.

Think about all the anatomy you have learned over the years. Think about all the taxonomy and how it was done: sometimes by thename of the discoverer and more often by its anatomical location. The abductor hallucis seems to be the latter.
The abductor and adductor hallicus function from approximately midstance to pre swing (1-4) (toe off), applying equal and opposite rotational vectors of force (in an ideal world) of the proximal phalynx of the hallux. This should resolve into a purely compressive force (5). In a closed chain environment, the transverse head of the adductor hallicus should act to prevent “splay” of metatarsals, along with the lumbricals and interossei (6), providing stabilzation of the forefoot (7) and rearfoot (8) during preswing, while the oblique head serves to help maintain the medial longitudinal arch.
The abductor hallicus is actually a misnomer, as it most cases it is not an abductor but rather a plantar flexor of the 1st ray, particularly the proximal hallux, (assisting the peroneus longus) and supinator about the oblique midtarsal joint axis (5). In the majority of cases, there doesn’t appear to be a separate, distinct insertion of the adductor hallicus to the base of the proximal phalynx, but rather a conjoint insertion with the lateral head of the flexor hallicus bevis into the lateral sesamoid and base of the proximal phalynx (9-11), emphasizing more of its plantar flexion function and stabilizing actions, rather than abduction.
In one EMG study of 20 people with valgus (12) they looked at activity of adductor and abductor hallucis, as well as flexor hallucis brevis and extensor hallucis longus. They found that the abductor hallucis had less activity than the adductor. No surprise here; think about reciprocal inhibition and increased activity of the adductor when the 1st ray cannot be anchoroed. They also found EMG amplitude greater in the abductor hallucis by nearly two fold in flexion.
So, the abductor hallucis seems to be important in abduction but more important in flexion. Either way, it is a stance phase stabilizer that we are beginning to know a lot more about. As for the name? You decide...
Dr Ivo Waerlop, one of The Gait Guys
1. Basmajian JV, Deluca CJ . Muscle Alive. Their Functions Revealed by Electromyography Williams and Wilkins. Baltimore, MD 1985, 377
2. Root MC, Orien WP, Weed JH. Normal and Abnormal Function of the Foot. Clinical Biomechanics, Los Angeles, CA 1977
3. Mann RA. Biomechanics of Running. In Pack RP. d. Symposium on the foot and leg in running sports. Mosby. St Louis, MO 1982:26
4. Lyons K, Perry J, Gronley JK. Timing and relative intensity of the hip extensor and abductor muscle action during level and stair ambulation. Phys Ther 1983: 63: 1597-1605
5. Michaud T. Foot Orthoses and Other Forms of Conservative Foot Care. Newton MA 1993: 50-55
6. Fiolkowski P, Brunt D, Bishop et al. Intrinsic pedal musculature support of the medial longitudinal arch: an electromyography study. J Foot & Ankle Surg 42(6) 327-333, 2003
7. Travell JG, Simons DG. Myofascial Pain and Dysfunction: The Trigger Point Manual. Williams and Wilkins, Baltimore 1992; 529
8. Kalin PJ, Hirsch BE. The origin and function of the interosseous muscles of the foot. J Anat 152, 83-91; 1987
9. Owens S, Thordarson DB. The adductor hallucis revisited. Foot Ankle Int. 2001 Mar;22(3):186-91. Am J Phys Med Rehabil. 2003 May;82(5):345-9.
10. Brenner E.Insertion of the abductor hallucis muscle in feet with and without hallux valgus. Anat Rec. 1999 Mar;254(3):429-34.
11. Appel M, Gradinger R. [Morphology of the adductor hallux muscle and its significance for the surgical treatment of hallux valgus][Article in German] Orthop Ihre Grenzgeb. 1989 May-Jun;127(3):326-30.
12. Arinci I, Geng H, Erdem HR, Yorgancioglu ZR Muscle imbalance in hallux valgus: an electromyographic study. Am J Phys Med Rehabil. 2003 May;82(5):345-9.
#halluxvalgus #halluxabductovalgus #bunion #footmuscleactivity #gait #thegaitguys
Minimalist. Maximalist. Neutral. Sometimes you need to earn your way into a shoe. After all, a shoe is supposed to direct and guide your foot to better (more optimal?) mechanics, not necessarily create more work for it. The literature seems to point to maximalist shoes changing lower extremity kinematics and increasing impact forces. The body needs to have the ability to “attenuate“ these impact forces, otherwise problems could potentially arise.
Take a good look at this gal. She is having a heck of a time trying to control what her mechanics are doing in this maximalist shoe. She demonstrates poor control of the foot, as well as the knee and hip.
By design, the shoe has a thicker outsole and forefoot flare (ie: The front of the shoe is wider at the sole than it is at the interface of the foot with it). This can create accelerated forefoot pronation as you see here with the medial aspect of the foot “slapping“ down on the ground. This creates a large valgus moment at the knee, which is further accentuated by her external tibial torsion, greater on the left. Also notice the pelvic dip on the left on the right foot hits the ground; less so on the right side when the left foot strikes. Looking up the chain and as a whole, you can see that this is poor control and could potentially contribute to at the mechanics at the ankle, knee and hip. Not sure if you can see it but she also has an increase in her lumbar lordosis, diminishing her ability to be able to use her abdominal core to help to stabilize.
If she were to continue to want to utilize the shoe, we would need to work on core strength, hip stability and most likely, forefoot motion (so that she can get her first ray complex to the ground at the first metatarsal phalangeal joint), before she “earns her way” into this shoe.
Dr Ivo Waerlop, one of The Gait Guys
Kulmala JP, Kosonen J, Nurminen J, Avela J.Running in highly cushioned shoes increases leg stiffness and amplifies impact loading. Sci Rep. 2018 Nov 30;8(1):17496. FREE FULL TEXT
Law MHC, Choi EMF, Law SHY, Chan SSC, Wong SMS, Ching ECK, Chan ZYS, Zhang JH, Lam GWK, Lau FOY, Cheung RTH. Effects of footwear midsole thickness on running biomechanics. J Sports Sci. 2019 May;37(9):1004-1010
Chan ZYS, Au IPH, Lau FOY, Ching ECK, Zhang JH, Cheung RTH. Does maximalist footwear lower impact loading during level ground and downhill running? Eur J Sport Sci. 2018 Sep;18(8):1083-1089.
Sinclair J, Richards J, Selfe J, Fau-Goodwin J, Shore H.The Influence of Minimalist and Maximalist Footwear on Patellofemoral Kinetics During Running.J Appl Biomech. 2016 Aug;32(4):359-64.
Chambon N, Delattre N, Guéguen N, Berton E, Rao G. Is midsole thickness a key parameter for the running pattern? Gait Posture. 2014;40(1):58-63
#runnning #gait #biomechanics #maximalistshoes #midsolethickness #gaitanalysis #thegaitguys
As I study this video more and more (yep, we just keep looking at things because we are that nerdy and that paranoid that we missed something) I saw at least 3 very subtle findings.
Watch the video of this right handed physical therapist who had L knee reconstruction (MCL/ACL with hamstring allograft) a few (hundred) times and see what you come up with, then come back and read this. We lie to slow things down and even frame by frame it with the slow motion feature or space bar to stop it. As background to the clinical exam, he has limited hip and knee extension on the left, 4/5 weakness of the quadratus femoris. His popliteus tests strong and 5/5. He has right sided back pain with L sided knee pain at the joint line and just inferior and medial. the treadmill is at a 2% grade at 2 mph.
Notice how he has a pelvic drift to the right during stance phase on that side. Why do you think? Remember, he has had a left sided knee surgery that left him with limited knee extension on that side. This creates a functional short leg on that side (the left), so he needs to get the longer (right) leg around. We don’t always see lateral movement of the pelvis on the longer leg side, but our guess is he is trying to “shorten” the longer leg side; lateral translation in the coronal plane is one strategy to accomplish that.
Now look at the left side. Can you see the subtle hip hike to clear the right leg? How about the small amount of circumduction? Sometimes folks will employ more than one strategy to get around a long leg, but ususally one will predominate, but not in this case.
Did you catch the abductory twist of the right heel? The longer leg side needs to go through a greater range of motion of ankle dorsiflexion which will store more potential energy in the tricep surae as well as long flexors of the toes, that energy needs to go somewhere!
Now think about step length. It will often be shortened on the shorter leg side. He still needs to move forward the same amount, so he uses the right arm to help propel his center of mass forward. Do you see the increased arm swing?
And why does he abduct his right arm so much? Where is his center of mass at left foot strike? It is all the way to the right, because of the “short leg”, correct? How can you counterbalance that? Abducting the arm would certainly accomplish that. Why does it go across the body? It is no longer needed to be that lateral during stance phase on the right, but he still needs to use it to propel himself forward with the shortened step length we talked about before.
Mental gymnastics, running through what runs through our minds and why things may appear the way that they do. A great lesson in knowing what is supposed to happen and when in the gait cycle
Dr Ivo Waerlop, one of The Gait Guys
#kneepain #lowbackpain #gaitanalysis #thegaitguys #visualgaitanalysis
I wrote a multipart series on Uner Tan Syndrome, the people who walk on all fours years ago. Recently there has been a video of a young lady walking and running on all 4 limbs, like some kind of cat or canine. It triggered me to put this article up again on the research and thoughts behind this quadruped gait in humans. It worth rewinding today. We have written and updated several of our, and Dr. Tan's, theories and thoughts on it from direct communication with Dr. Tan. You can search for all the parts under "uner tan" in the search box.
"From the viewpoint of dynamic systems theory, it was concluded there may not be a single factor that predetermines human quadrupedalism in Uner Tan syndrome, but that it may involve self-organization, brain plasticity, and rewiring, from the many decentralized and local interactions among neuronal, genetic, and environmental subsystems."
Full Blog post here:
https://www.thegaitguys.com/…/the-hand-walkers-the-family-t…
The hand walkers: The family that walks on all fours. Part 1
Quadrupedalism and its commentary on human gait. To understand your athlete, your patient, your client, whatever your profession, you need to have a good understanding of neurodevelopment. If your client has some functional movement pattern flaws it could be from a delayed or expedited neurodevelopmental window. Generalized training and rehab will not correct an early or late window issue; often your work must be more specific.
When we began our journey into our daily writings on “The Gait Guys blog” we had no idea of the never ending tangents our writing would take pertaining to gait, human movement and locomotion. It has become plainly obvious over time that this blog will likely exist as long as we choose to continue it.
In 2006 we saw a documentary documentary entitled The Family That Walks On All Fours LINK: https://www.youtube.com/watch?v=ef3eKj4Pivk&feature=youtu.be
. . . and the video clip is from the documentary. It was a fascinating documentary and with our backgrounds in neurology, neurobiology, neuroscience, biomechanics and orthopedics we had more questions than the documentary touched upon. The documentary opened up many thoughts of neuro-development since we all start with a quadrupedal gait. But there had to be more to it than just this aspect because people eventually move through that neurologic window of development into bipedial gait. This has been in the back of our minds for many years now. Today we will touch upon this family and their challenges in moving through life, today we talk about Uner Tan syndrome, Unertan syndrome or UTS.
The original story is about the Ulas family of nineteen from rural southern Turkey. Tan described five members as walking with a quadrupedal gait using their feet and the palms of their hands as seen in this video. The affected family members were also severely mentally retarded and displayed very primitive speech and communication. Since his initial discovery several other families from other remote Turkish villages have also been discovered. In all the affected individuals dynamic balance was impaired during upright walking, and they habitually chose walking on all four extremities. Tan proposed that these are symptoms of Uner Tan syndrome.
UTS is a syndrome proposed by the Turkish evolutionary biologist Uner Tan. Persons affected by this syndrome walk with a quadrupedal locomotion and are afflicted with primitive speech, habitual quadrupedalism, impaired intelligence. Tan postulated that this is a plausible example of “backward evolution”. MRI brain scans showed changes in cerebellar development which you should know after a year of our blog reading means that balance and motor programming might be thus impaired. PET scans showed a decreased glucose metabolic activity in the cerebellum, vermis and, to a lesser extent the cerebral cortex in the majority of the patients. All of the families assessed had consanguineous marriages in their lineage suggesting autosomal recessive transmission. The syndrome was genetically heterogeneous. Since the initial discoveries more cases have been found, and these exhibit facultative quadrupedal locomotion, and in one case, late childhood onset. It has been suggested that the human quadrupedalism may, at least, be a phenotypic example of reverse evolution.
Neurodevelopment of Children:
Children typically go through predictable windows of neurodevelopment. Within a set time frame they should move from supine to rolling over. Then from prone they should learn to press up into a push up type posturing which sets up the spine, core and lower limbs to initiate the leg movements for crawling. Once crawling ensues then eventual standing and cruising follow. In some children, it is rare yet still not neurodevelopmentally abnormal, they move into a “bear crawl” type of locomotion where weight is born on the hands and feet (just as in our video today of UTS). Sometimes this window comes before bipedalism and sometimes afterwards but it should remain a short lived window that is progressed through as bipedalism becomes more skilled.
In studying Uner Tan Syndrome, Nicholas Humphrey, John Skoyles, and Roger Keynes have argued that their gait is due to two rare phenomena coming together.
“First, instead of initially crawling as infants on their knees, they started off learning to move around with a “bear crawl” on their feet.Second, due to their congenital brain impairment, they found balancing on two legs difficult.Because of this, their motor development was channeled into turning their bear crawl into a substitute for bipedalism.”
According to Tan in Open Neurol, 2010
It has been suggested that the human quadrupedalism may, at least, be a phenotypic example of reverse evolution. From the viewpoint of dynamic systems theory, it was concluded there may not be a single factor that predetermines human quadrupedalism in Uner Tan syndrome, but that it may involve self-organization, brain plasticity, and rewiring, from the many decentralized and local interactions among neuronal, genetic, and environmental subsystems.
There is much more we want to talk about on this mysterious syndrome and the tangents and ideas that come from it. We will do so in the coming weeks as we return to this case. We will talk about other aspects of neurodevelopment which should be interesting to you all since most our readers either are having children, will have them, or are watching them move through these neurologic windows. And we know that some of our readers are in the fields of therapy and medicine so this should reignite some thoughts of old and new. In future posts we will talk about cross crawl patterning in the brain, bear crawling, the use of the extensor muscles in upright posture and gait as well as other aspects of neurodevelopment gone wrong. We are not even close to being done with this video and all of its tangents. In the weeks to come we hope you will remain interested and excited to read more about its deep implications into normal and abnormal human gait.
author: Dr. Shawn Allen, one of the gait guys
References:
Open Neurol J.
2010 Jul 16;4:78-89. Uner tan syndrome: history, clinical evaluations, genetics, and the dynamics of human quadrupedalism.
Tan U
.Department of Physiology, Çukurova University, Medical School, 01330 Adana, Turkey.
link: http://www.ncbi.nlm.nih.gov/pubmed/21258577
Humphrey, N., Keynes, R. & Skoyles, J. R. (2005).
“Hand-walkers: five siblings who never stood up”
(PDF).
Discussion Paper
. London, UK: Centre for Philosophy of Natural and Social Science.
http://informahealthcare.com/…/abs/10.1080/00207450701667857
http://informahealthcare.com/…/abs/10.1080/00207450500455330
http://www.ncbi.nlm.nih.gov/pubmed…
https://www.youtube.com/watch?v=ef3eKj4Pivk&feature=youtu.be
Here it is, in all its glory...Our version of the short foot exercise. Love it or hate it, say it “doesn’t translate”, we find it a useful training tool for both the patient/client as well as the clinician. It awakens and creates awareness of the sometimes dormant muscles in the user and offers a window to monitor progression for them, as well as the observer.
Remember that the foot intrinsics are supposed to be active from midstance through terminal stance/pre swing. Having the person “walk with their toes up” to avoid overusing the long flexors is a cue that works well for us. This can be a useful adjunct to your other exercises on the road to better foot intrinsic function.
Dr Ivo Waerlop, one of The Gait Guys
Sulowska I, Mika A, Oleksy Ł, Stolarczyk A. The Influence of Plantar Short Foot Muscle Exercises on the Lower Extremity Muscle Strength and Power in Proximal Segments of the Kinematic Chain in Long-Distance Runners Biomed Res Int. 2019 Jan 2;2019:6947273. doi: 10.1155/2019/6947273. eCollection 2019
Okamura K, Kanai S, Hasegawa M, Otsuka A, Oki S. Effect of electromyographic biofeedback on learning the short foot exercise. J Back Musculoskelet Rehabil. 2019 Jan 4. doi: 10.3233/BMR-181155. [Epub ahead of print]
McKeon PO, Hertel J, Bramble D, et al. the foot core system: a new paradigm for understanding intrinsic foot muscle function Br J Sports Med March 2014 doi:10.1136/bjsports-2013- 092690
Dugan S, Bhat K: Biomechanics and Analysis of Running Gait Phys Med Rehabil Clin N Am 16 (2005) 603–621
Bahram J: Evaluation and Retraining of the Intrinsic Foot Muscles for Pain Syndromes Related to Abnormal Control of Pronation http://www.aptei.ca/wp-content/uploads/Intrinsic-Muscles-of-the-Foot-Retraining-Jan-29-05.pdf
#shortfootexercise #footexercises #footrehab #thegaitguys #gaitanalysis #gaitrehab #toesupwalking
https://vimeo.com/342800960
tag/key words: gait, gaitproblems, gaitanalysis, forefootrunning, forefootstrike, heelstrike, pronation, central fatigue, peripheral fatigue, fatigue, hip rotation, gait biomechanics, running
Links to find the podcast:
Look for us on iTunes, Google Play, Podbean, PlayerFM, Radio.com and more.
Just Google "the gait guys podcast".
Our Websites:
www.thegaitguys.com
Find Exclusive content at: https://www.patreon.com/thegaitguys
doctorallen.co
summitchiroandrehab.com
shawnallen.net
Our website is all you need to remember. Everything you want, need and wish for is right there on the site.
Interested in our stuff ? Want to buy some of our lectures or our National Shoe Fit program? Click here (thegaitguys.com or thegaitguys.tumblr.com) and you will come to our websites. In the tabs, you will find tabs for STORE, SEMINARS, BOOK etc. We also lecture every 3rd Wednesday of the month on onlineCE.com. We have an extensive catalogued library of our courses there, you can take them any time for a nominal fee (~$20).
Our podcast is on iTunes and just about every other podcast harbor site, just google "the gait guys podcast", you will find us.
Where to find us, the podcast Links:
iTunes page:
https://itunes.apple.com/us/podcast/the-gait-guys-podcast/id559864138?mt=2
Google Play:
https://play.google.com/music/m/Icdfyphojzy3drj2tsxaxuadiue?t=The_Gait_Guys_Podcast
Direct download URL: http://traffic.libsyn.com/thegaitguys/pod_1488_-_61419final.mp3
Permalink URL: http://thegaitguys.libsyn.com/podcast-a-deep-dive-case-study-plus-central-and-peripheral-fatigue-explained
Libsyn Directory URL: http://directory.libsyn.com/episode/index/id/10151672
Folks with femoral retro torsion often experience lower back pain with twisting movements
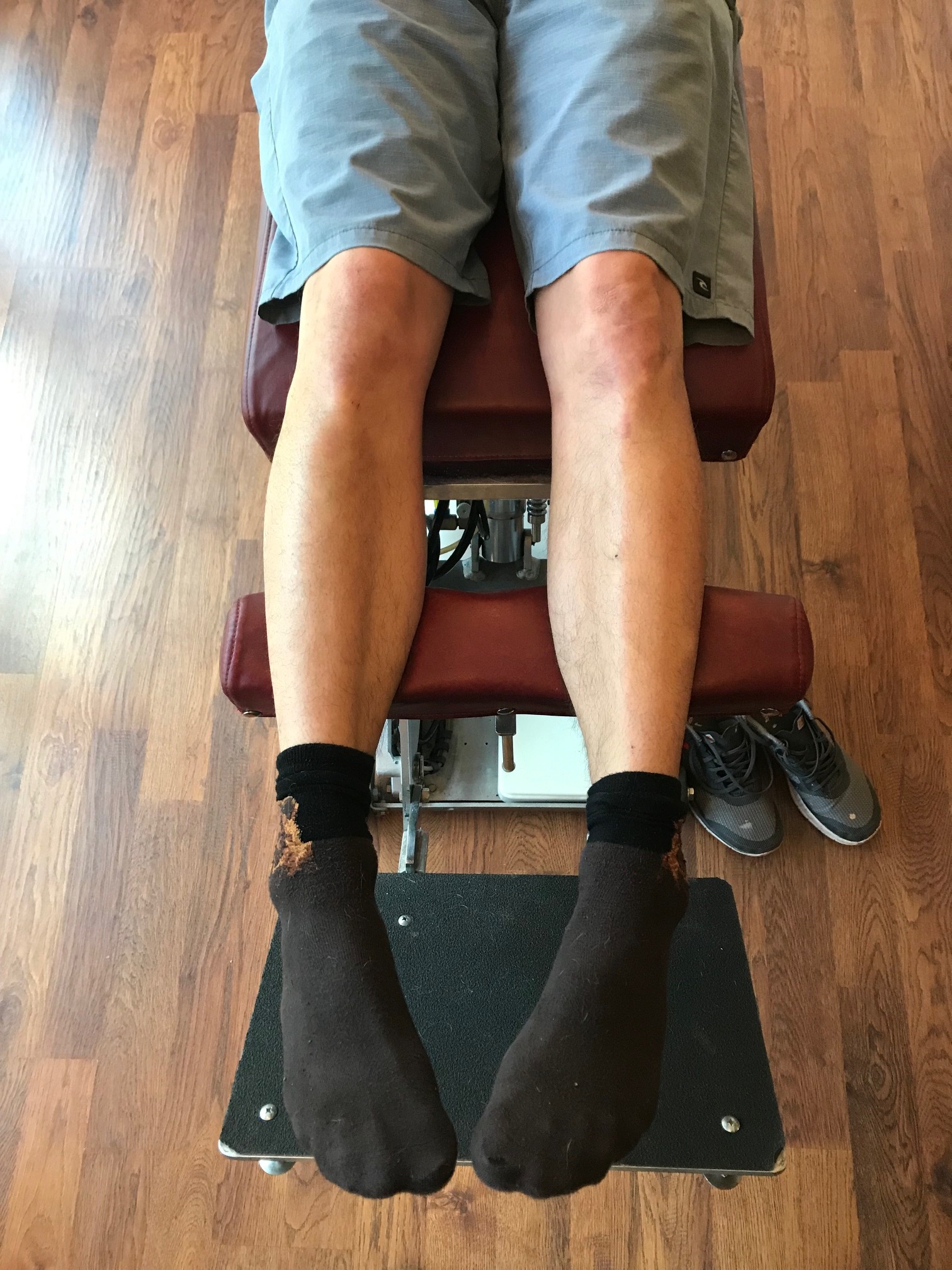
This left handed hydrology engineer Presented to the office with an acute onset of lower back pain following “swinging a softball bat”. He comments that he always “hit it out of the park“ and hit “five home runs“ in the last game prior to his backs demise.

note the internal tibial torsion. drop a plumbline from the tibial tuberosity. it should pass through the 2nd met or between the 2nd and 3rd met shafts

note the internal tibial torsion. drop a plumbline from the tibial tuberosity. it should pass through the 2nd met or between the 2nd and 3rd met shafts
He presented antalgic with a pelvic shift to the left side, flexion of the lumbar spine with 0° extension and a complete loss of the lumbar lordosis. He could not extend his lumbar spine past 0° and was able to flex approximately 70. Lateral bending was approximately 20° on each side. Neurological exam negative. Physical exam revealed bilateral femoral retro torsion as seen above. Note above the loss of internal rotation at the hips of both legs, thus he has very limited internal rotation of the hips. Femoral retroversion means that the angle of the neck of the femur (also known as the femoral neck angle) is less than 8°, severely limiting internal rotation of the hip and often leading to CAM lesions.
Stand like you’re in a batters box and swing like you’re left handed. What do you notice? As you come through your swing your left hip externally rotates and your right hip must internally rotate. He has no internal rotation of the right hip and on a good day, the lumbar spine has about 5° of rotation with half of that occurring at the lumbosacral junction. Guess what? The facet joints are going to become compressed!
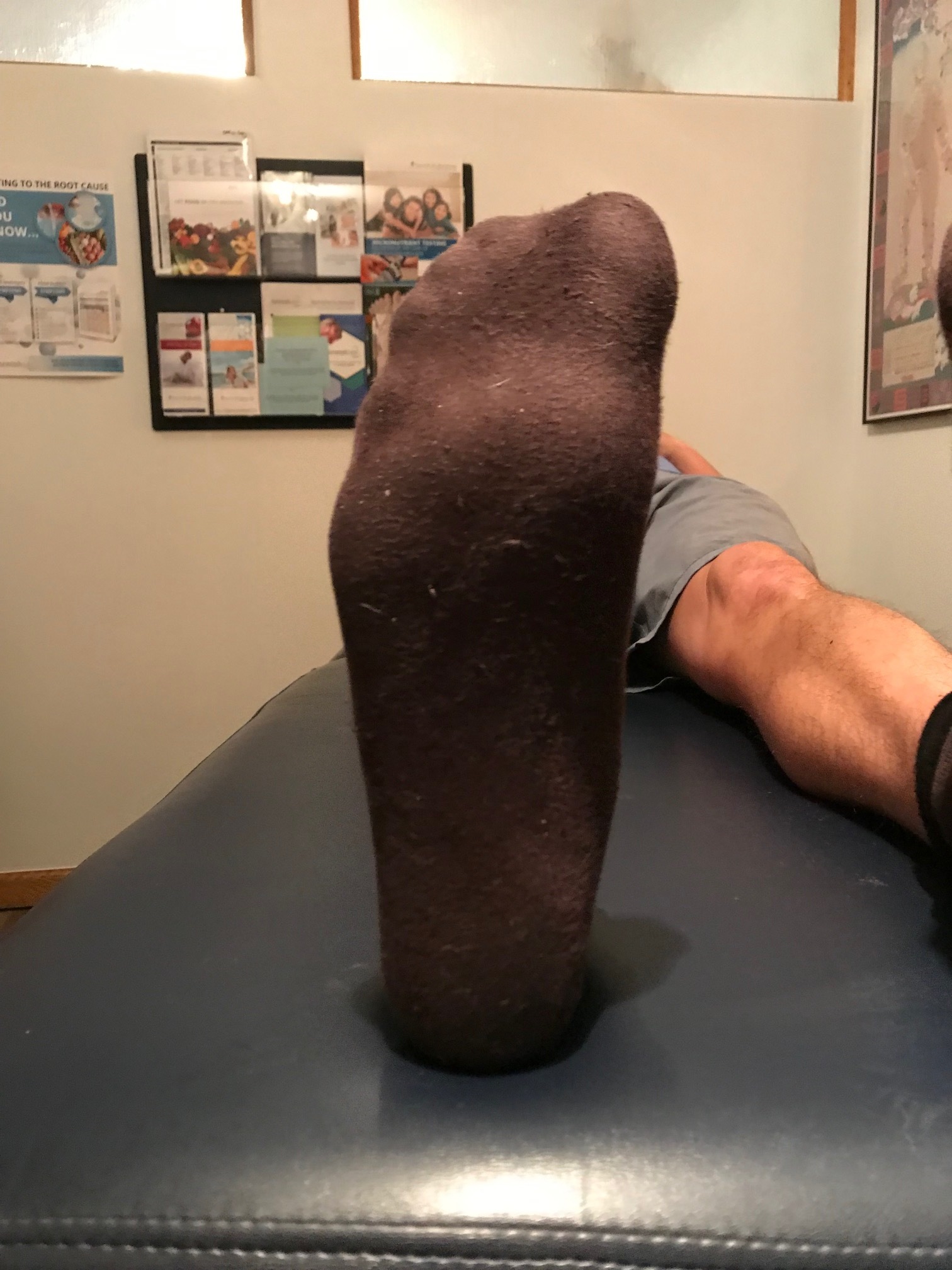
bisect the calcaneus. the line should fall though the 2nd metatarsal or between the 2nd and 3rd met shafts

bisect the calcaneus. the line should fall though the 2nd metatarsal or between the 2nd and 3rd met shafts
Now combine that with bilateral 4 foot adductus (see photos above). His foot is already in supination so it is a poor shock observer.
Go back to your “batters box“. Come through your swing left handed. What do you notice? The left foot goes into a greater amount of pronation in the right foot goes into a greater amount of supination. Do you think this is going to help the amount of internal rotation available to the hip?
When folks present with lower back pain due to twisting injuries, make sure to check for femoral torsions. They’re often present with internal tibial torsion, which is also present in this individual.
Remember a while ago we said “things occur in threes”. That goes for congenital abnormalities as well: in this patient: femoral retro torsion, internal tibial torsion and forefoot adductus.
What do we do? Treat locally to reduce inflammation and take steps to try to improve internal rotation of the hips bilaterally as well as having him externally rotate his right foot when he is in the batteries box to allow him to "create" more internal rotation of the right hip.
Dr Ivo Waerlop, one of The Gait Guys
#internalrotation #hipproblem #femoraltorsion #femoralversion #retroversion #retrotorsion #thegaitguys

Of course this article is not exclusive for sprinters, it pertains to any running sport, even endurance.
Maximum isometric force had increased by 49% and tendon CSA by 17% !
Tendons can change their cross sectional area, if you load them.
Here I show lateral forefoot loading in a heel raise, and a medial forefoot loading in heel raise. This has to be part of the discovery process outlined below. Forefoot types will play into the loading choice, and unequal strength of the medial or lateral calf compartment will also play into the loading choice made. Where do you need to put your strength ? And is the forefoot competent to take that loading challenge ? Meaning, do they have a forefoot valgus? A forefoot supinatus ? These things matter. If you are a sprinter, how you load the forefoot bipod might be a variable of foot type, asymmetrical posterior compartment strength, or foot strike pattern in the frontal plane (search our blog for cross over gait and glute medius targeting strategies for step width) ,or a combination of several or all of the above. These things matter, and why and where you put your strength matters, if you are even aware of where and how you are putting the loads, and why of course. Of course, then there are people like the recent Outside online article that says how you foot strike doesn’t matter, but it does matter. But of course, if you do not know the things we have just mentioned, it is easy to write such an article.
Isometrics are useful, they have their place. In a recent podcast we discussed the place and time to use isometrics, isotonics, eccentrics and concentrics.
One of the goals in a tendinopathy is to restore the tendon stiffness. Isometrics are a safe way to load the muscle tendon complex without engaging a movement that might have to go through a painful arc of movement. With isometrics here is neurologic overspill into the painful arc without having to actually go there.
The key seems to be load. More load seems to get most people further along. Remember, the tendon is often problematic because it is inflammed and cannot provide a stiffness across its expanse. Heavy isometric loading seems to be a huge key for most cases. But, we have to say it here, not everyone fits this mold. Some tendons, in some people, will respond better to eccentrics, and strangely enough, some cases like stretching (perhaps because this is a subset of an eccentric it seems or because there is a range of motion issue in the joint that is a subset of the problem). Now the literature suggests that stretching is foolish, but each case is unique all in its own way, and finding what works for a client is their medicine, regardless of what the literature and research says.
Finding the right load for a given tendon and a right frequency of loading and duraction of loading is also case by case specific. Part of finding the right loading position is a discovery process as well, as noted in the photos above. Finding the fascicles you want to load, and the ones you do not want to load (painful) can be a challenging discovery process for you and your client. Finding the right slice of the pie to load, and the ones not to load takes experimentation. When it is the achilles complex, finding the safe However, if one is looking for a rough template to build from, brief, often, heavy painfree loads is a good template recipe to start with.
Here, in this Geremia et al article, "ultrasound was used to determine Achilles tendon cross-sectional area (CSA), length and elongation as a function of plantar flexion torque during voluntary plantar flexion."
They discovered that, "At the end of the training program, maximum isometric force had increased by 49% and tendon CSA by 17%, but tendon length, maximal tendon elongation and maximal strain were unchanged. Hence, tendon stiffness had increased by 82%, and so had Young’s modulus, by 86%.
Effects of high loading by eccentric triceps surae training on Achilles tendon properties in humans. Jeam Marcel Geremia, Bruno Manfredini Baroni, Maarten Frank Bobbert, Rodrigo Rico Bini, Fabio Juner Lanferdini, Marco Aurélio Vaz
European Journal of Applied Physiology
August 2018, Volume 118, Issue 8, pp 1725–1736

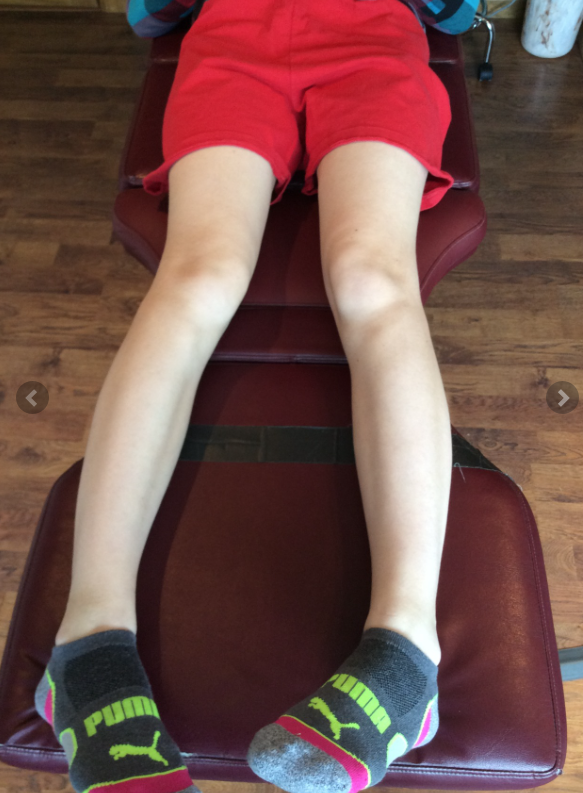
In the 1st picture note this patient is in a neutral posture. Note how far externally rotated her right foot is compared to the left. Note that when you drop a plumbline down from the tibial tuberosity it does not pass-through or between the second and third metatarsals. Also note the incident left short leg

In the next picture both of the patients legs are fully externally rotated. Note the large disparity from right to left. Because of the limited extra rotation of the right hip this patient most likely has femoral retro torsion. This means that the angle of her femoral head is at a greater than 12° angle. We would normally expect approximately 40° of external Rotation. 4 to 6° is requisite for normal gait and supination.
In the next picture the patients knees are fully internally rotated you can see that she has an excessive amount of internal rotation on the right compare to left, confirming her femoral antetorsion.

When this patient puts her feet straight (last picture), her knees point to the inside causing the patello femoral dysfunction right greater than left. No wonder she has right-sided knee pain!
Because of the degree of external tibial torsion (14 to 21° considered normal), activity modification is imperative. A foot leveling orthotic with a modified UCB, also inverting the orthotic is helpful to bring her foot somewhat more to the midline (the orthotic pushes the knee further outside the sagittal plane and the patient internally rotate the need to compensate, thus giving a better alignment).
a note on tibial torsion. As the fetus matures, The tibia then rotates externally, and most newborns have an average of 0- 4° of internal tibial torsion. At birth, there should be little to no torsion of the tibia; the proximal and distal portions of the bone have little angular difference (see above: top). Postnatally, the tibia should twist outward (externally) a total of 15 degrees until adult values are reached between ages 8 and 10 years of 23° of external tibial torsion (range, 0° to 40°).
Wow, cool stuff, eh? Dr Ivo Waerlop, one of The Gait Guys
#tibialtorsion #tibialversion #kneepain #thegaitguys #gaitanalysis
Just some more thoughts for those who insist on coaching arm swing changes.
"Whole-body coordination patterns may become partitioned in particular ways as a function of task requirements.”
Toddlers actively reorganize their whole body coordination to maintain walking stability while carrying an object. Hsu WH1, Miranda DL2, Chistolini TL3, Goldfield EC4. Gait Posture. 2016 Oct;50:75-81
Today we seem to be going back to dual-tasking again, in this case utilizing the arms as balance assistance devices, amongst their other functions. However, we all know that walking with a hand in a pocket, or carrying something alters our ability to maximize their ballast-like function. Balanced walking involves freely swinging the limbs in pendullar motion. Changes in arm swing will change gait economy and efficiency. We have all run with a water bottle or bag/briefcase and know how that changes the symmetry and fluidity of our gait.
Today's research piece discusses toddlers and their function as they carry objects. "children immediately begin to carry objects as soon as they can walk. One possibility for this early skill development is that whole body coordination during walking may be re-organized into loosely coupled collections of body parts, allowing children to use their arms to perform one function, while the legs perform another. Therefore, this study examines: 1) how carrying an object affects the coordination of the arms and legs during walking, and 2) if carrying an object influences stride length and width." -Hsu et al.In this study of 10 toddlers with 3-12 months of walking experience were recruited to walk barefoot while carrying or not carrying a small toy. "Stride length, width, speed, and continuous relative phase (CRP) of the hips and of the shoulders were compared between carrying conditions. While both arms and legs demonstrated destabilization and stabilization throughout the gait cycle, the arms showed a reduction in intra-subject coordination variability in response to carrying an object. Carrying an object may modify the function of the arms from swinging for balance to maintaining hold of an object. The observed period-dependent changes of the inter-limb coordination of the hips and of the shoulders also support this interpretation. Overall, these findings support the view that whole-body coordination patterns may become partitioned in particular ways as a function of task requirements." -Hsu et al.
So once again we will say it, if you are coaching the arm swing YOU want, because you do not like what you see in your client, or if you think you are helping your client get more out of their body in terms of speed, power, efficiency or anything of the sort, know that there is a higher, smarter program running the show. And that program in the client’s CNS is smarter than you when it comes to what they need for whole-body coordination pattern generation.
Remember the popliteus? To recap, it contracts at the initial contact phase of the walking gait cycle, to act as an accessory PCL (look HERE
https://www.thegaitguys.com/search?q=popliteus&f_collectionId=57d4982c91b18610c6ee3e0f
to read about that), then contracts eccentrically to slow the rate of internal rotation of the femur on the tibia until midstance, so as not to macerate the meniscus; It then contracts concentrically to accelerate the external rotation of the femur on the tibial plateau so it rotates faster then the tibia, to protect the meniscus as well. So, internal rotation of the femorotibial complex from initial contact to midstance and external rotation of the complex from midstance to preswing. Got it?
Now look at the video of this gal with L sided medial knee pain and past history of a left tibial plateau fracture in her youth. Do you see it? Hmmmm; doesn’t look like internal rotation does it? Don’t see it? Remember that the whole complex SHOULD be internally rotating until the swing phase leg passes the stance pase leg. See it now? Considering that the popliteus tested weak on the clinical exam, does this surprise you?
Agreed that there are many factors initiating internal rotation (and thus pronation) of the stance phase leg from initial contact to midstance, like plantar flexion, adduction and eversion of the talus, contraction of the lower leg anterior compartment muscles, eccentric contraction of the quads and hamstrings, just to name a few, can you see how (a least theoretically) one bad player can ruin the team?
Yes, popliteus rehab, along with abdominal core and foot core endurance exercises are in her future.
Dr Ivo Waerlop, one of The Gait Guys
#popliteus #kneepain #kneeproblem #thegaitguys #gaitanalysis
For those arm swing/pulsers/ COM and head over foot folks consider some more research below.
Let the CNS drive the show, it is what it is there for . . . The leg motor patterns are dominant, the arms are passive and "shape" and influence the leg swing as a balance and ballast effect. As we discuss in an upcoming podcast, to cross the arms in a pumping motion across the midline of the body means one has to have compromised scapular mechanics (mostly protraction) to afford that much humeral adduction. This means we are forcing thoracic rotation as well. This means we are reversing what we know is more true, that "arm motion is driven passively by rotation of the thorax (Pontzer et al., 2009), an idea which is supported by shoulder muscle EMG data" (and not thoracic rotation by arm swing). Why would we try to create more unnatural axial spin through the spine when we are actually trying to move forward in the sagittal plane? Why would we try to force more rotation through the spine when the function of the thoracopelvic canister (ie. the core) is to stabilize rotational /angluar momentum? Hmmmm, things to ponder.
"Previous modelling studies have clearly shown that motion of the arms effectively counterbalances the angular momentum of the lower extremities during running (Hamner & Delp, 2013; Hamner et al., 2010). It has further been suggested that arm motion is driven passively by rotation of the thorax (Pontzer et al., 2009), an idea which is supported by shoulder muscle EMG data, consistent with the shoulders as spring-like linkages (Ballesteros, Buchthal, & Rosenfalck, 1965). Our data are con- sistent with this idea, showing motion of the thorax to be in the opposite direction to that of the swinging leg. Pontzer et al. (2009) also suggested that motion of the thorax is driven passively by motion of the pelvis. However, our data shows that the thorax reaches its peak angular velocity earlier than the pelvis, indicating that thorax motion is not completely passively driven by pelvic movements."
-S.J. Preece et al. / Human Movement Science 45 (2016) 110–118

image credit: https://pixabay.com/vectors/slide-sliding-falling-stickman-151861/
A single event can generate asynchronous sensory cues due to variable encoding, transmission, and processing delays. Robert Peterka talks about this, along with posture compensation and system apportionment when it comes to balance and coordination of the visual, vestibular and proprioceptive systems. We have talked about that here on the blog in the past.
We are often looking for ways to “highlight” pathology and make it more visible in the clinical exam. Having your patient/client walk backwards is one of those tools.
Walking and remaining upright in the gravitational plane requires 3 integrated systems to work in concert with one another: the visual, vestibular and proprioceptive systems. Backwards walking requires a more coordinated effort AND IF there is a “hiccup” or extra demand on the system (the proprioceptive in this case), neurological processing can take a little longer, efforts can be delayed and the end result is a greater compensation is needed; this often makes pathology more evident.
Try having your client walk backwards when you are doing your exam and see what we mean. We think you will be surprised with the results : )
Dr Ivo Waerlop, one of The Gait Guys
Peterka RJ, Statler KD, Wrisley DM, Horak FB. Postural compensation for unilateral vestibular loss. Front Neurol. 2011 Sep 6;2:57. doi: 10.3389/fneur.2011.00057. eCollection 2011.
temporal Shayman CS, Seo JH, Oh Y, Lewis RF, Peterka RJ, Hullar TE.Relationship between vestibular sensitivity and multisensory temporal integration. J Neurophysiol. 2018 Oct 1;120(4):1572-1577. doi: 10.1152/jn.00379.2018. Epub 2018 Jul 18.
Hawkins KA, Balasubramanian CK, Vistamehr A, Conroy C, Rose DK, Clark DJ, Fox EJ. Assessment of backward walking unmasks mobility impairments in post-stroke community ambulators. Top Stroke Rehabil. 2019 May 12:1-7. doi: 10.1080/10749357.2019.1609182. [Epub ahead of print]
#backwardwalking #clinicalexam #thegaitguys #gaitpathology #clinicaltricksofthetrade

We get “help me” emails from all over the world on a regular basis. Recently we received this photo from a runner in Oxford, UK, often we cannot help, but when there is a story to tell that everyone can learn from, we offer what we can. This runner was frustrated, explaining a “dodgy foot”. We like the word.
dodg·y däjē/
-dishonest or unreliable; potentially dangerous; of low quality.
We can likely guarantee you that the solution here to this runner’s form issue is not wholly at the foot which appears “in toed” and slanted and appears ready to kick the back of the right heel, not to mention the knees that are about to brush together. Thus, merely working on their foot strike would be so remedial and corrupt that it would a crime.
Ivo and I do not take on cases via the internet because we cannot give all the information because we cannot examine the client, many do offer such services but people are not being given the whole story and we pledged long ago not to be part of the problem. Anyone who recommends exercises from things they see on a video gait analysis are basically doing the same disservice in our opinion. But sometimes, as in this case, their inquiry offers a opportunity for dialogue. This is one of those cases. I will not be presenting a solution, because I do not have the examination information I need, but I will propose a thought process that further investigation may afford progress towards some answers.
This appears like a non-pathologic cross over gait in my mind until proven otherwise, there may be other sources, causes and components, but when it quacks like a duck you’d be silly not to check for webbed feet. There are many component parts that leave someone with a cross over type gait (ie a narrow based gait, that if taken further, might as well result in running on a line). This runner even confirmed upon questioning that the left foot scuffs the inside of the right ankle/shin often, both sides scuff in fact but more left shoe on right shin. No Einsteinian epiphany there.
This means a narrow swing through (adducting) left limb.
This might mean stance and swing phase gluteus medius communication problems.
This might mean swing leg foot targeting problems.
This often suggests right, but sometimes both right and left, frontal plane pelvis sway problems which means pelvis control is challenged which means core lumbar stability control is challenged.
This means adaptive arm swing changes from the clean norm. Arm swing to a large degree is driven by the lower limb motor patterns, despite what some people will propose (dive into our archives to find some of those research articles).
This does NOT mean this runner has pain, or pain yet, or maybe never will have pain but there are many determinants of that which I will discuss below.
But, make no mistake, this is flawed gait mechanics, but that does not translate to injury, speed, outcome or pain. But when they come with those complaints attached, one would be foolish not to at least consider these biomechanics as a source.
The left swing leg is clearly targeting a more medial placement, meaning limb adduction (active or passive or both is to be determined) and this is a product of the cross over gait (unfamiliar with the cross over gait ? SEARCH our blog for the term, you will need a few hours of free time to get through it all). Some would call the cross over gait a lazy gait, but I would rather term it an efficient gait taken too far that it has now become a liability, a liability in which they can no longer stabilize frontal plane sway/drift. A wider gait on the other hand, as in most sprinters, is less efficient but may procure more power and the wider base is more stable affording less frontal plane drift. Just go walk around your home and move from a very narrow line walking gait to a wide gait and you will feel a more powerful engagement of the glutes. Mind you, this is not a fix for cross over gaits, gosh, if it was only that simple !
This runner might investigate whether there is right frontal plane drift, and if it is in fact occurring, find the source of the drift. It can come from many places on either limb. (This client says they are scuffing both inside ankles, which is not atypical and so we likely have drift on both right and left). We have discussed many of them here in various places on the blog over the years. Now as for “Why” the foot looks in toed, well that can also come from many places. Quite simply the adducted limb once it leaves toe off (a toe off that is most often a "low gear toe off", meaning not a medial/hallux toe off), can look like this. But, perhaps it is also a product of insufficient external rotation maintenance occurred during that left stance phase, affording more internal rotation which is being unchecked and observed here during early swing. Remember though, if this is in fact a cross over gait result, in this gait the limb approaches the ground unstacked (foot is too far inside a left hip joint plumb line) the foot will greet the ground at a far lateral strike and in supination. Pronation will thus be magnified and accelerated, if there is enough time before toe off. However, and you can try this on your own by walking around your home, put yourself in terminal stance at toe off. Make sure you have the foot inverted so you are toeing off the lateral toes (low gear toe off). Does this foot not look like the one in the photo ? Yes it does, now just lift the foot off the ground and you have reproduced this photo. And when combined with a right pelvis drift, the foot will sneak further medially appearing postured behind the right foot.
Keep this in mind as well, final pronation and efficient hallux (big toe) toe off does often not occur in someone who strikes the ground on a far lateral foot. I am sure this runner will now be aware of how poorly they toe off of the big toe, the hallux. They will tend to progress towards low gear toe off, off the lesser toes. This leaves the foot inverted and this is what you are seeing in her the photo above. That is a foot that is inverted and supinated and it carried through all the way through toe off and into early swing. It is a frequently component of the cross over gait, look for it, you will find it, often.
Final thoughts, certainly this can be an isolated left swing phase gluteus medius weakness enabling an adducted swing limb thus procuring a faulty medial foot placement, but it is still part of the cross over phenomenon. Most things when it comes to a linked human frame do not work in isolation. But i will leave you with a complicating factor and hopefully you will realize that gait analysis truly does require a physical exam, and without it you could be missing the big picture problem. What if she has a notable fixed anatomic internal tibia torsion on that left side. Yup, it could all be that simple, and that is not something you can fix, you learn to manage that one as a runner.
* Side bar rant: Look at any google search of runners photos and you will see this type of swing limb foot posturing often, far too often. That does not mean it is normal ! That means, that many people do this, but it cannot mean that it is optimal mechanics. And yes, you can take the stance that “I do it as well and i have no injuries or problems so what is the big deal?”. Our response is often “you do have an issue, it may be anatomic or functional, but you do have an asymmetrical gait and you think it is not a problem, YET”. And maybe you will run till you are 6 feet under and not have a problem because you have accommodated over many years and you are a great compensator, yes, some people get lucky. Some people also do not run enough miles that these issues express themselves clinically so lets be fair. But some of these people are reality deniers and spend their life buying the newest brace or gadget, trying a different shoe insert, orthotic or new shoe of the month and shop over and over again for another video gait analysis expert who can actually fix their pain or problem. And then there are those who have a 45 minute home exercise program that they need to do to keep their problems at bay, managing, not fixing anything. Or, they spend an hour a week on the web reading article after article on what are the top 4 exercises for iliotibial band syndrome for example. They shop for the newest Graston practitioner, the newest kinesio taping pattern, Voodoo bands, breathing patterns, compression socks etc. And sometimes they are the ones that say they still don't have a problem.You get the drift. Gosh darn it, find someone who knows what the hell they are doing and can help you fix the issues that are causing the problem. And yes, some of the above accoutrements may be assistive in that journey.
I have dealt with this unique toe off issue very frequently. Once you see something enough times, you learn all of the variations and subtle nuances that a problem can take on. But, trying to fit everyone into a similar solution model is where the novice coach, trainer or clinician will get into trouble. Trust us, it all starts with an examination, a true clinical physical examination. If one leaves the investigatory process to a series of screens or functional movement patterns, “activation” attempts, digital gait analysis or strength tests one is juggling chainsaws and the outcome you want is often not likely to occur. There is nothing wrong with making these components part of the investigation process, but on their own, they are not enough to get the honest answer many times. Of course, Ivo and i were not able to jump the pond and examine this runner with our own eyes and hands so today’s dialogue was merely to offer this runner some food for thought to open their mind to our thought process, in the hopes that they can find someone to help them solve the underlying problem and not merely make the gait look cleaner. Making someone’s walking or running gait look cleaner is not hard, but making it subconsciously competent and clean (without thought or effort) requires a fix to the underlying problem. We can ALMOST guarantee you that the solution here to this runner’s form issue is not wholly at the foot that looks in toed and slanted. Merely working on their foot strike would be so remedial and corrupt that it would a crime.
Dr. Shawn Allen, one of the gait guys
#gait, #gaitproblems, #crossovergait, #gaitanalysis, #gluteweakness, #toeoff
This 54-year-old pilot presented to our office with pain on the outside of his right knee while cycling with his wife who is currently training for the triple bypass. The discomfort comes on later in the ride and is largely lateral. He thought it may be due to a seat position so he raised his seat up but then shortly developed lower back discomfort. Lowered the seat back down and presents to the office today. He is currently on a 54 cm Pierello road bike with a straight top tube.
Physical exam revealed him to have moderately limited internal rotation of the right hip which was approximately 5 degrees external rotation; left side had approximately 5 degrees of internal rotation. There was no significant leg length discrepancy or internal tibial torsion. Musculature, save for the long extensors the toes tests 5/5 and strong. Hip extension is 0 degrees bilaterally 5 flexion approximately 120 degrees with tightness mostly in the iliopsoas and some in the rectus femoris. Knee stability tests are unremarkable. Some patellofemoral discomfort with compression on the right. Palpable tightness in the right IT band.
X-rays revealed degenerative changes at the inferior aspect of the right acetabulum with a small spur an osteophyte formation.
His seat height was set so that at bottom dead center with the seat tube he had a 30 degree bend in his knee. Seat fore and aft position placed the knee over pedal spindle behind central axis of the pedal. His pedal stroke, seen on the video, reveals moderate internal rotation and medial displacement of the knee on the right side.
So what is going on?
It’s all about how folks compensate. This gent has very limited internal rotation of the right hip. Due to the nature of cycling, he is REALLY TRYING to get his 1st MTP down to the pedal to generate power. This is not unusual among cyclists, which is why what you think should be happening in gait does not always transfer over to cycling. in doing so, he MUST rotate SOMETHING forward (in this case his pelvis) medially to create the internal rotation needed. From this scenario, you can see how the posturing would increase knee valve and offer a mechanical advantage to the vastus lateralis, causing patello femoral dysfunction and knee pain.
So we did we do?
Moved his seat forward so that a line drawn from between the patella and tibial tuberosity fell through the center axis of the pedal
Angled his cleat so that he is able to have a greater progression angle moving forward, bringing his knee more into the sagittal plane
Began working on the hip to increase internal rotation working on the gluteus minimus, vastus lateralis and biceps femoris as well as hip capsule and ilio/ischio/pubofemoral ligaments
Dr Ivo Waerlop, one of The Gait Guys
#kneepain #cycling #hipproblem #femoralretrotorsion #thegaitguys #torsion
OUR SEARCH BOX IS INTUITIVE, TYPE IN YOUR KEY WORD, WAIT, THEN SCROLL DOWN.
Email us: our email is found under the "Disclaimer" Tab above.
Powered by Squarespace.