Part 2: The Turning: The thoracic spine in connecting the kinetic chain
/Yesterday I provided a blog post on this photo here. Today I want to pose a rabbit hole for you to ponder, in the hopes that you see how much deeper this process is at looking at gait and locomotion . . . . . thoracic rotation.
Below you will find yesterdays post, if you read it yesterday you can scroll down to the *** down below and read what I ask you to ponder today (but its always nice to review :)
From yesterday's blog post:
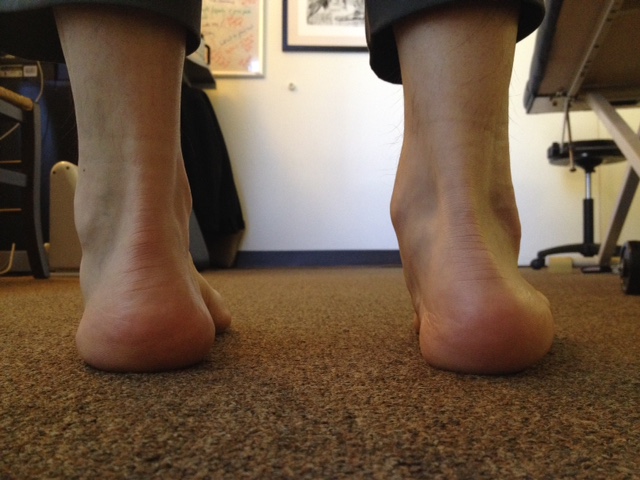
"It should be simple and clear in the photo that I am turning my neck and thoracic spine strongly to the left. The left rotation has forced me to find stability over the lateral left foot while driving the rotation with the right foot. Left foot had to supinate, right had to pronate. No rocket science here.
Earlier in the week I posted a brief discussion on the neck and proprioception and the upper and lower limb. I caught some questions on challenging the strength of the neurological linkages to the lower limb, so I promised a simple picture to solidify my point.
Where is what i wrote earlier this week.
"From the study: "Limb proprioception is an awareness by the central nervous system (CNS) of the location of a limb in three-dimensional space and is essential for movement and postural control. The CNS uses the position of the head and neck when interpreting the position of the upper limb, and altered input from neck muscles may affect the sensory inputs to the CNS and consequently may impair the awareness of upper limb joint position."
We say it is not just the upper limb however, the neck and head posture is used in interpreting the position of the lower limb as well. And similarly altered head/neck muscle input can impair awareness of the lower limb posture as well. Think about it, we are trying to stay upright in the gravitational plane while keeping the eyes and vestibular centers on the horizon. Gait is nothing more than a single leg balancing act repeated over and over. Faulty info on where our center of pressure is from a visual or vestibular aspect will alter where we put our foot in space. Just look at how many neurologic diseases end up with a wider based gait, because our proprioceptive centers no longer trust our base of support. It is all connected."
Exp Brain Res. 2015 May;233(5):1663-75. doi: 10.1007/s00221-015-4240-x. Epub 2015 Mar 13.Neck muscle fatigue alters upper limb proprioception. Zabihhosseinian M1, Holmes MW, Murphy B.
As in this study, and putting it together with my photo and discussion at the start here today, limb proprioception is an awareness by the CNS of the location of the limb and is essential for proper movement and postural control. If I had rotated to the left and had my CNS not known where the foot was in space and in relation to the rest of my body, I may have fallen over to the left. Instead, my CNS sensed the weight shift to the left from the neck and torso rotation, and moved my foot weight bearing into supination (affording a slightly greater lateral weight bearing on the foot) to accommodate the shift in my center of pressure and mass laterally. So, the CNS used the position of the head and neck, and the weight shift, in interpreting the appropriate positioning of the lower limbs. Sometimes moving the foot into supination to accommodate the lateral load is not enough, and we need to actually step laterally to maintain upright. Altered input from my neck muscles might affect the sensory inputs to the CNS and consequently may impair the awareness of my limb joint positioning in space. This happens often in vestibular challenged clients and in client of aging decline where the system is losing proprioception. If we do not know where a body part is in space, we don't know how to use it or how to load it (think about chronic ankle sprains).
As i said earlier this week, think about it, we are trying to stay upright in the gravitational plane while keeping the eyes and vestibular centers on the horizon. Gait is nothing more than a single leg balancing act repeated over and over. Faulty info on where our center of pressure is from a visual or vestibular aspect will alter where we put our foot in space. Just look at how many neurologic diseases end up with a wider based gait, because our proprioceptive centers no longer trust our base of support. It is all connected.
Think about how amazing this system is when it works right, we can run on a track leaning into the curve, we can ride a bike and lean into turns, we can run forward and yet turn to look behind us, all without falling over -- thanks to our CNS and joint proprioception.
*** Today, to build on the above principles, adding the concept of thoracic rotation and even more, scapular stability, breathing, rib cage and thoracic spine mobility and stability, specifically thoracic rotation is critical. What if any of these movements are lost in this client's turning attempt ? Let's keep it simple, what if thoracic rotation is lost, specifically what if the client has lost left thoracic rotation? What happens then to the left foot in this scenario ? Can they achieve enough left foot supination to achieve enough left lateral weight shift to make up for the loss of left thoracic rotation ? Can they achieve enough of these movements without exceeding the tipping point at the ankle creating an inversion sprain? For the task to be completed, the motion is going to occur somewhere, the question is, will the place it occurs be a safe place ?
Lets complicate things further, and ask about hip rotation, what if the left hip has impaired internal rotation, after all it is part of the left turning pattern. At the terminal end range of thoracic rotation in this case, any further rotation needs will come from hip internal rotation typically (once the pelvis stops spinning leftward with the spine rotation). What if that hip rotation end range is impaired or limited ? Something has to give, the turning goal is defined, the question remains does the client have the working parts to get the turning done without overloading any single area causing pathology ? Furthermore, the right foot must be able to perform the requisite pronation and external hip rotation for similar reasons during the turning. Sharp directional change cutting sports like soccer, basketball and football all require this kind of motion, namely the discussed cervical rotation, thoracic rotation, hip rotation and ability to stabilize safely on a supinated foot at times. For example, try running downfield at a full clip and suddenly look and turn back over your left shoulder to catch a football pass, these are the component parts I just outlined above. If any of them are limited or missing we can see injury, whether its a torn ACL, hip impingement, sprained ankle, neck or shoulder strain etc. Everything i have outlined in the last 3 blog posts has to be clean and with safe sensory-motor patterning. The problem is, we teach people to run and catch, but we often do not look at these component parts as I have discussed looking for limitations, potential places were these glitches harbor. These are the component things and frameworks of thinking and problem solving that I do in my office. I hope you do think the same way as well, we can be friends then :)
The next time your client comes in with an ankle inversion sprain, or hip pain, or shoulder or thoracic pain just as examples, try asking them about what they were doing at the time of the event. Work backwards from there and see if they had the component parts or if one was missing that could be the culprit.
I had a client just this past week during the NYC marathon invert his ankle when he looked back to snap a selfie with the crowd behind him. What i discussed today was the likely mechanism -- his thoracic rotation to that side sucked when I examined him and he had loss of internal hip rotation on that side. The motion had to go somewhere , sadly it was one degree of ankle supination too much this time. Many injuries do not occur in a vacuum, there is a reason if you know how to think it through and examine the parts -- go beyond your movement screenings though, it is just a piece of the pie. Oh, one more thing, if this was your client and all you did was begin managing his ankle sprain and nothing else, well, you are just a technician, and you are better than that. Your job is to find the problems within the system, not the compensations which often only show up in movement screens, you must examine your client. You must see if they are neurologically intact, determine if there are weaknesses, compensations, shortness, tightness, endurance issues, skill issues, joint range limitations, aberrant movement patterns amongst other things. You must find these things, then you must figure out why they are there, then you must begin to remedy them.
Dr. Shawn Allen, the other gait guy