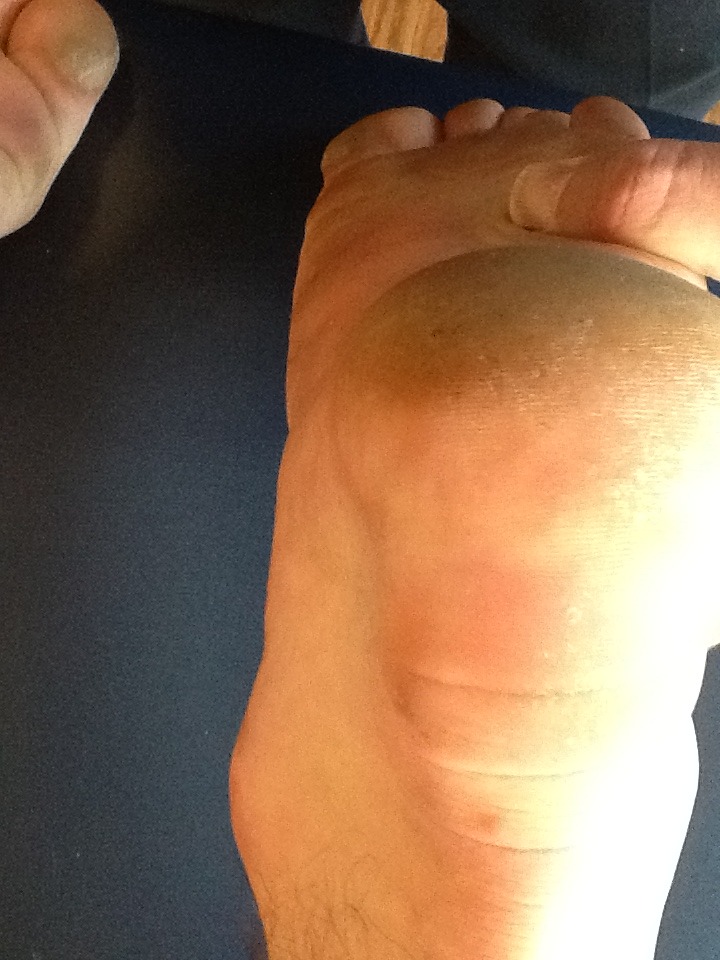
What do we have here and what type of shoe would be appropriate?
/You are looking at a person with a fore foot varus. This means that the fore foot (ie, plane of the metatarsal heads) is inverted with respect to the rear foot (ie, the calcaneus withe the subtalar joint in neutral). Functionally translated, this means that they will have difficulties stabilizing the medial tripod (1st MET head) to the ground making the forefoot and arch unstable and likely rendering the rate and degree of pronation increased.
The incidence of this condition is 8% of 116 female subjects (McPoil et al, 1988) and 86% of 120 male and female subjects (Garbalosa et al, 1994), so it seems to happen happen more in males. We think this second number is inflated and those folks actually had a forefoot supinatus, which is much more common.
Fore foot varus occurs in 3 flavors:
- compensated
- uncompensated
- partially compensated
What is meant by compensated, is that the individual is able to get the head of the 1st ray to the ground completely (compensated), partially, or, when not at all, uncompensated.What this means from a gait perspective ( for partially and uncompensated conditions) is that the person will pronate through the fore foot to get the head of the 1st ray down and make the medial tripod of the foot (ie, they pronate through the subtalar joint to allow the 1st metatarsal to contact the ground). This causes the time from mid-stance to terminal stance to lengthen and will inhibit resupination of the foot.
Today we are looking at a rigid, uncompensated forefoot varus, most likely from insufficient talar head derotation during fetal development and subsequent post natal development. They will not get to an effective foot tripod. They will collapse the whole foot medially. These people look like severely flat-footed hyperpronators.
So, what do you do and what type of shoe is appropriate? Here’s what we did:
- try and get the 1st ray to descend as much as possible with exercises for the extensor hallucis brevis and short flexors of the toes (see our videos on youtube)
- create more motion in the foot with manipulation, massage mobilization to optimize what is available
- strengthen the intrinsic muscles of the feet (particularly the interossei)
- increase strength of the gluteus maximus and posterior fibers of the gluteus medius to slow internal rotation of the leg during initial contact to midstance
- put them in a flexible shoe for the 1st part of the day, to exercise the feet and a more supportive; medially posted (ideally fore foot posted) shoe for the latter part of the day as the foot fatigues
- monitor his progress at 3-6 month intervals
- a rigid orthotic will likely not help this client and they will find it terribly uncomfortable because this is a RIGID deformity for the most part (the foot will not accommodate well to a corrective orthotic. Besides, the correction really has to be made at the forefoot anyways.
Lost? Having trouble with all these terms and nomenclature? Take our national shoe fit program, available by clicking here.
The Gait Guys. Uber foot geeks. Separating the wheat from the chaff, with each and every post.