The loads are going to go somewhere.
/You cannot change one thing, and not expect the other parts to change, to have to adapt, and possibly those parts to complain at some point.
The loads are going to go somewhere.
Too much pronation means the arch may be reduced in height, but it also means that the first ray complex (the 1-2 metatarsals essentially) is dorsiflexing more than normal. This means they will not likely get to their adequate plantarflexion by the time the foot is ready to heel rise and toe off at supination. In other words, if you have pronated and dorsiflexed too long and too much, you will eat up the time you needed to plantarflex and supinate.
This means that "Increased foot pronation may compromise ankle plantarflexion moment during the stance phase of gait, which may overload knee and hip."-Resende et al
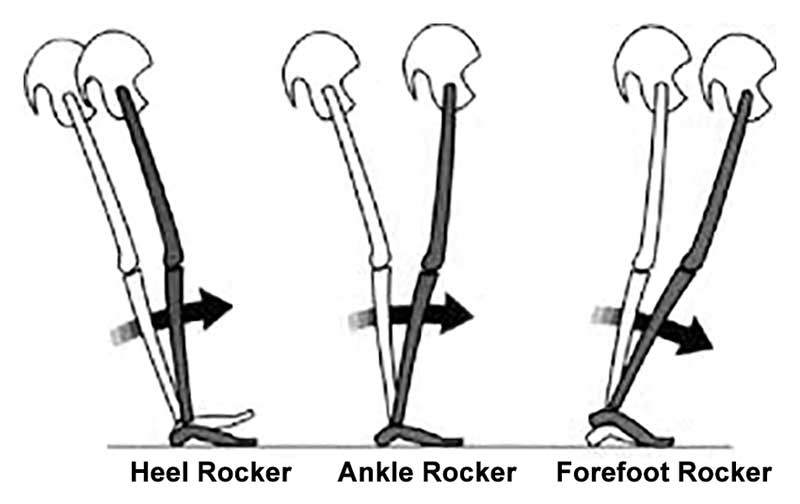
If you cannot plantarflex the foot-ankle complex sufficiently, or in a timely manner, you should understand that you are carrying this fault forward while moving into heel rise during the forefoot rocker stance phase of gait, and you are doing it over a less stable, less rigid foot-ankle complex because it is still in relative pronation. This means you are placing higher propulsive loads over an unprepared ankle-foot complex. This means different/altered posterior compartment function, which can mean altered knee and hip function. Sagittal plane function, to name the most obvious, will have to create and endure compensatory loads. Sure, they may be fine for a time, but perhaps there will be a cost over time. Now, many might say, "if it is not a problem now, it is not a problem", let them build robustness on their chosen pattern; that can be very hopeful and shortsighted thinking in our opinion. Why not change things that are obviously aberrant and build robustness on a pattern and correction that is suspected to be more sound? This can be a cyclical argument that no one wins, EVER, we all see it all the time. After all, the arguments become silly after time, and we resist our own silly comments like "well, why change the oil in your car right now, nothing bad is happening at this time. Or, well that front right tire, though bald and nearly flat, is still rolling along so why bother changing it out?" But that stuff gets no one anywhere, other than pissed off, so we hold back. The debate never gets furthered along, because no one can see the future.
So, we will leave this rant with this thought, we cannot change one thing, and not expect the other parts to change, have to adapt. And adaptation can be both good OR bad. Or maybe we should say, good AND bad.
The loads are going to go somewhere. Lets leave it at that.
photo: credit pixabay.com
Gait Posture. 2018 Oct 23;68:130-135. doi: 10.1016/j.gaitpost.2018.10.025. [Epub ahead of print]
Effects of foot pronation on the lower limb sagittal plane biomechanics during gait.
Resende RA1, Pinheiro LSP2, Ocarino JM3.