Botox for plantar fasciitis? Sounds like a bad idea to us....
/image source: https://commons.wikimedia.org/wiki/File:Plantar_aponeurosis_-_axial_view.png
Botox..For plantar fasciitis? Really?
We found this article (1) in one of our favorite journals, Lower Extremity Review , and were a little surprised. Let us get this straight: you are going to take one of the the most poisonous biological neurotoxins known (1) and inject it into your calf and foot?
The article in LER is well written and the results (thankfully) were inconclusive regarding its usage. They do cite 3 studies (with two by the same lead author) where it has been effective (2-4). Yes, it is better than saline (5) (but not as good as extracorporeal shock wave therapy (6)), and better than placebo (7-10) but considerably more risky.
So the premise is “if the muscle is dysfunctional, then let’s just take it out of the equation”. But this really doesn’t fix the problem, it just covers up the symptom. And what about the other potential side effects since botulinum toxin acts not only at the neuromuscular junction, blocking the release of acetylcholine, but also at the autonomic ganglia, postganglionic parasympathetic nerve endings, as well as the post ganglionic sympathetics that use acetylcholine (capillaries of skin, piloerector muscles and sweat glands) (11)?.
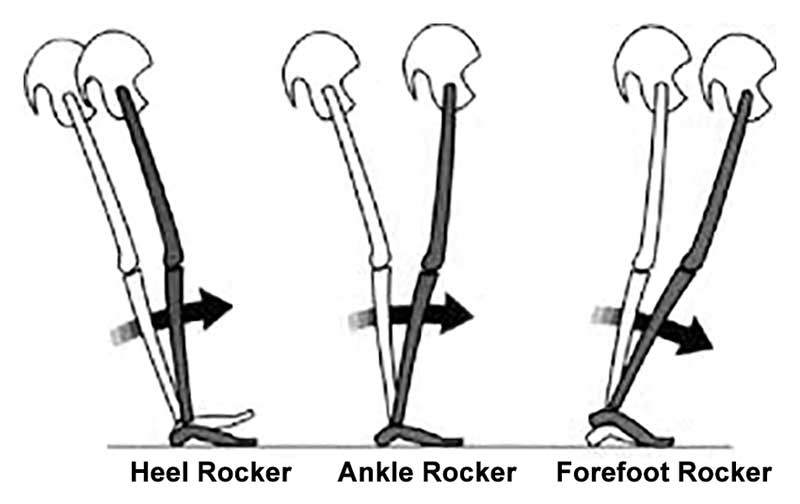
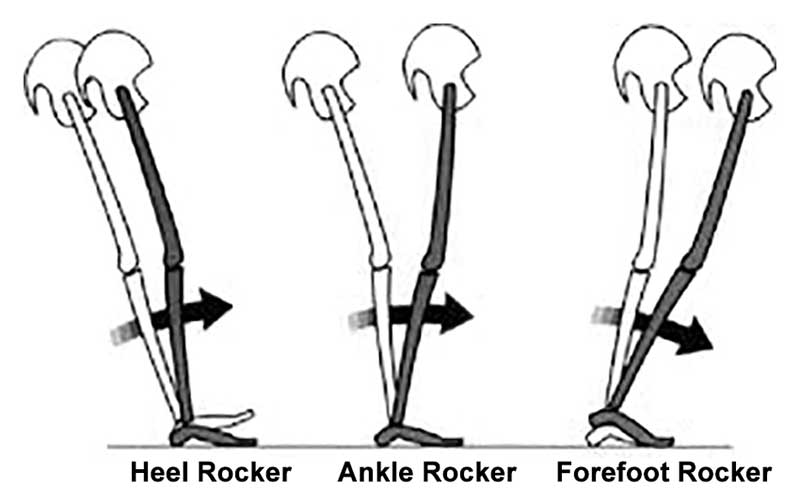
In our experience, most cases of plantar fasciitis are secondary to lack of forefoot rocker, lack of ankle rocker, lack of hip extension or in some cases, direct trauma. Wouldn’t it make more sense to strengthen the anterior compartment to reciprocally inhibit the posterior compartment, increasing ankle dorsiflexion and hip extension? We find, oftentimes, treating only the area of chief complaint and not what is "driving the bus" can offer temporary, symptomatic relief but not long standing pathmechanics or pathoanatomy.
Just like the road to enlightenment, there are no shortcuts in treating plantar fasciitis and if you are not going to treat the cause, then be prepared to reap what you sow.
Dr Ivo Waerlop, one of The Gait Guys
#botox #plantarfascitis #badideas #gaitproblem #thegaitguys
1. https://lermagazine.com/article/botox-injection-not-just-for-celebrities-furrows-and-wrinkles
2. Elizondo-Rodriguez J, Araujo-Lopez Y, Moreno-Gonzalez JA, Cardenas-Estrada E,
Mendoza-Lemus O, Acosta-Olivo C. A comparison of botulinum toxin A and intralesional steroids for the treatment of plantar fasciitis: A randomized, double-blinded study. Foot Ankle Int.
2013;34(1):8-14.
3. Díaz-Llopis IV, Rodríquez-Ruíz CM, Mulet-Perry S, Mondéjar-Gómez FJ., Climent-Barberá JM., Cholbi-Llobel F. Randomized controlled study of the efficacy of the injection of botulinum toxin type A versus corticosteroids in chronic plantar fasciitis: results at one and six months. Clin Rehabil. 2012;26(7):594-606.
4. Díaz-Llopis IV, Gómez-Gallego D, Mondéjar-Gómez FJ, López-García A, Climent-Barberá JM, Rodríguez-Ruiz CM. (2013). Botulinum toxin type A in chronic plantar fasciitis: clinical effects one year after injection. Clin Rehabil. 2013;27(8):681-685.
5. Ahmad J, Ahmad SH, Jones K. Treatment of Plantar Fasciitis With Botulinum Toxin. Foot Ankle Int. 2017 Jan;38(1):1-7. doi: 10.1177/1071100716666364. Epub 2016 Oct 1.1.
6. Roca B, Mendoza MA, Roca M. Comparison of extracorporeal shock wave therapy with botulinum toxin type A in the treatment of plantar fasciitis. Disabil Rehabil. 2016 Oct;38(21):2114-21. doi: 10.3109/09638288.2015.1114036. Epub 2016 Mar 1
7. Babcock MS, Foster L, Pasquina P, Jabbari B. Treatment of pain attributed by plantar fasciitis with botulinum toxin A: a short-term randomized, placebo-controlled, double blinded study. Am J Phys Med Rehabil. 2005;84(9):649-654.
8. Samant PD, Kale SY, Ahmed S, Asif A, Fefar M, Singh SD. Randomized controlled study comparing clinical outcomes after injection botulinum toxin type A versus corticosteroids in chronic plantar fasciitis. Int J Res Orthop. 2018;4(4):672-675.
9. Huang YC, Wei SH, Wang HK, Lieu FK. Ultrasonographic guided botulinum toxin type A treatment for plantar fasciitis: an outcome-based investigation for treating pain and gait changes. J Rehabil Med. 2010;42(2):136-140.
10. Ahmad J, Ahmad SH, Jones K. Treatment of plantar fasciitis with botulinum toxin. Foot Ankle Int. 2017;38(1):1-7.
11. Nigam PK, Nigam A. Botulinum toxin. Indian J Dermatol. 2010;55(1):8–14. doi:10.4103/0019-5154.60343