3 things
/Its subtle, but hopefully you see these 3 things in this video.
I just LOVE the slow motion feature on my iPhone. It save me from having to drag the video into Quicktime, slow it down and rerecord it.
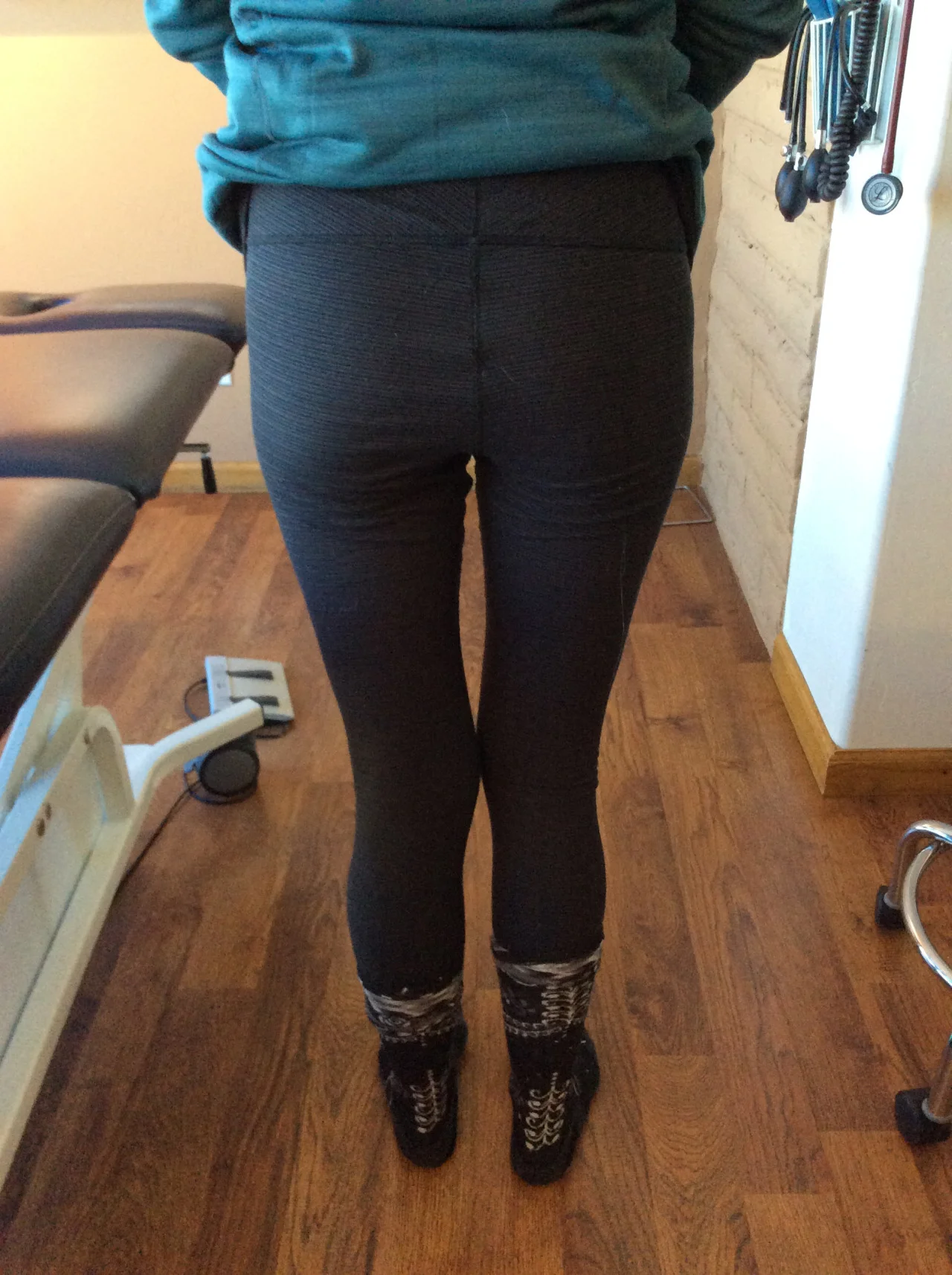
This gal has a healing left plantar plate lesion under the 2nd and 3rd mets. She has an anatomical leg length deficiency, short on the left, and bilateral internal tibial torsion, with no significant femoral version. Yes, there are plenty of other salient details, but this sketch will help.
1st if all, do you see how the pelvis on her left dips WAY more when she lands on the right? There is a small amount of coronal plane shift to the right as well. This often happens in gluteus medius insufficiency on the stance phase leg (right in this case), or quadratus lumborum (QL) deficiency on the swing phase leg (left in this case) or both. Yes, there are other things that can cause this and the list is numerous, but lets stick to these 2 for now. In this case it was her left QL driving the bus.
Watch the left and right forefeet. can you see how she strikes more inverted on the left? this is a common finding, as the body often (but not always) tries to supinate the shorter extremity (dorsiflexion, eversion and adduction, remember?) in an attempt to “lengthen” it. Yes, there is usually anterior pelvic tilt accompanying it on the side, because I knew you were going to ask : )
Look how her knees are OUTSIDE the saggital plane and remain there in her running stride. This is commonly seen in folks with internal tibial torsion and is one of the reasons that in our opinion, these folks should not be put medially posted, torsionally rigid, motion control shoes as this usually drive the knees FURTHER outside the saggital plane and can macerate the meniscus.
Yep, lots more we could talk about on this video, but in my opinion, 3 is a good number.
Dr Ivo Waerlop, one of The Gait Guys
#thegaitguys #gaitanalysis #footpain #gaitproblem #internaltibialtorsion #quadratuslumborum #footstrike
https://vimeo.com/329212767