Neuromechanics Weekly: How does appropriate movement diminish pain?
We talk about proper (or should we say appropriate) movement (including gait) inhibiting or diminishing pain. So, how does that happen?
Above on the left is a great diagram that we will work through.
You are looking at a cross section of a spinal cord (We can hear the groans already!) We remember that the dorsal horn (posterior part) is sensory and the ventral horn (front) is motor. In between them (the lateral horn) is autonomic (this runs automatized body functions such as your heart, lung, guts, etc).
Small nerve fibers subserve pain. These are the A delta and C nerve fibers. “Small” refers to fiber diameter of the nerve. These nerves are where pain stimuli enters the spinal cord; they enter the sensory dorsal horn and synapse/connect there with the next neuron in line that takes the sensory message up the spinal cord to the brain to tell you about the pain including its intensity, location etc. Pain can result from tissue damage or injury (which can be due to, or the result of, poor biomechanics).
Large diameter nerve fibers subserve sensations like touch, pressure, vibration, muscle spindles (muscle length) and golgi tendon organs (muscle tension/load). These fibers also enter the sensory dorsal horn, but they do not synapse immediately, unlike pain fibers. They ultimately travel up to the top of the brainstem or cerebellum to coordinate information with other data your brain is processing. They send a branch (or collateral) to an inhibitory neuron, which excites the inhibitory neuron. Thus, if you excite an inhibitory neuron, it does it’s job and inhibits the propagation of an impulse. In this case, it inhibits the pain impulse from traveling to the cortex. So pain is inhibited. Appropriate biomechanics excite the largest population of receptors and provide the most effective response.
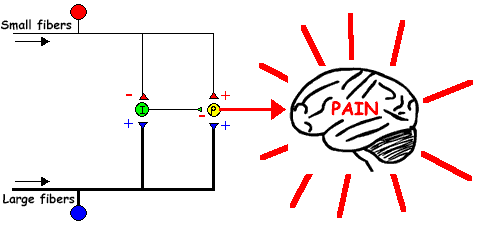
Now look at the diagram on the right. It is a simplified schematic of the one on the left, with detail of the connections. Note that the LARGE FIBERS (from joint mechanoreceptors, spindles, muscles, etc) EXCITE the inhibitory interneuron (which would inhibit it). Also note that the SMALL FIBERS INHIBIT the inhibitory internuron (which would excite it!)
There you have it. Clear as mud? Go through some of our old posts on receptors and FEEL THE PAIN (parts 1, 2, 3+4) and come back to this and read it again. You know you want to be a geek, so go ahead!
The Gait Guys: Geeks on many levels. helping you to presynaptically inhibit pain on a daily basis, through better movement.