Spanking the orthotic: The effects of hallux limitus on the foot’s longitudinal arch.
But the issues do not stop at the arch. If you have been with us long enough, you will have read about the effects of the anterior compartment (namely the tibialis anterior, extensor digitorum and hallucis and peroneus tertius muscles) strength and endurance on the arch.
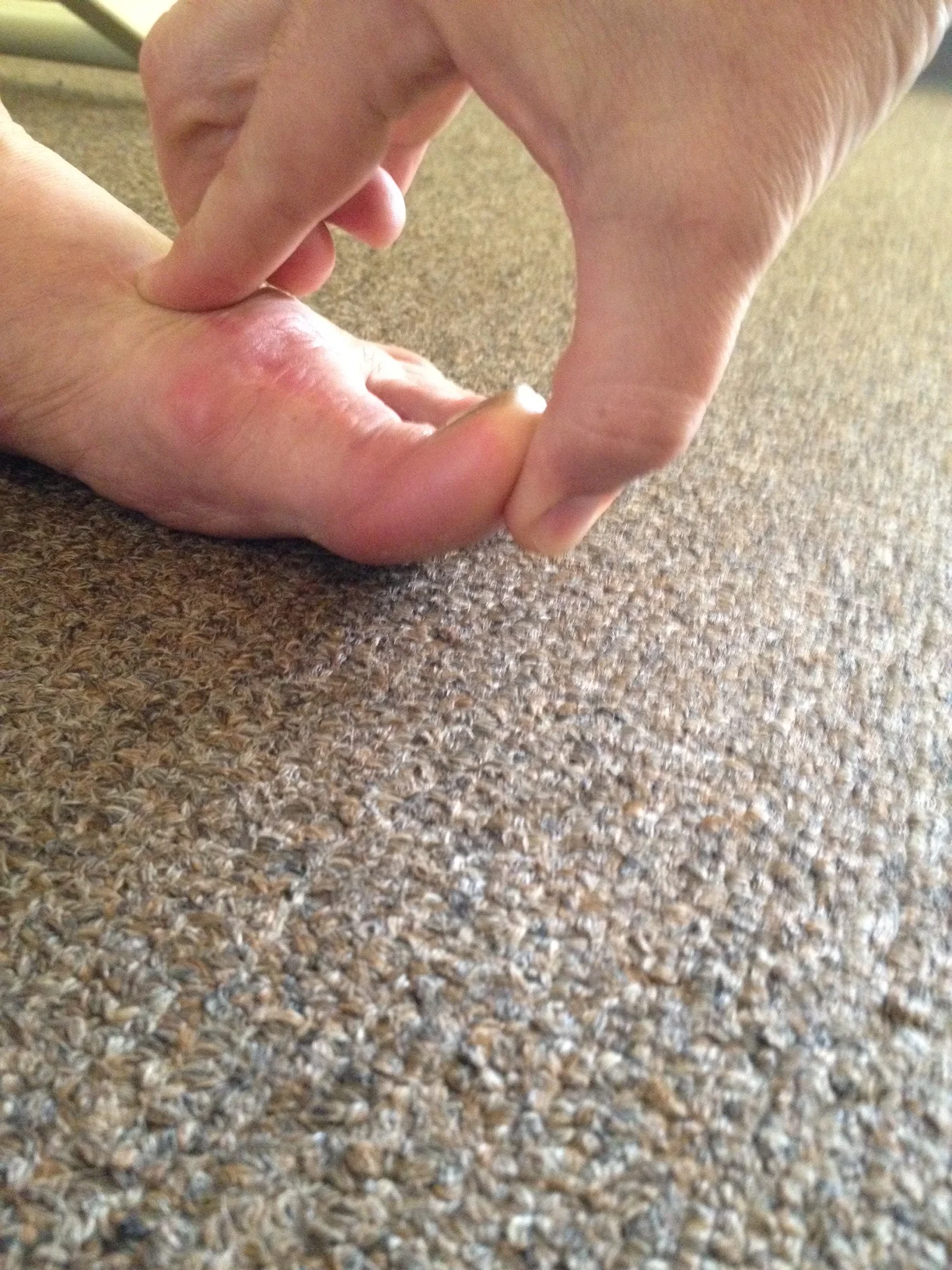
Here we have a very troubled foot. This foot has undergone numerous procedures, sadly. Today we will not talk about the hallux varus you see here, a virtual unicorn in practice (and acquired in this case) nor do we want to discuss the phalangeal varus drift. We want to draw your attention to the obvious impairment of the 1st MTP (metatarsophalangeal joint) dorsiflexion range. You can see the large dorsal crown of osteophytes, a dorsal buttress to any hallux dorsiflexion. There is under 10 degrees of dorsiflexion here, not even enough worth mentioning. We have said it many times before, if you lose a range at one joint usually that range has to be accommodated for proximal or distal to the impaired joint. This is a compensation pattern and you can see it here in the hallux joints themselves.
Here you can see that some of the dorsiflexion range has been acquired in the proximal phalangeal joint. We like to call this “banana toe” when explaining it to patients, it is a highly technical term but you are welcome to borrow it. This occurred because the joint was constantly seeing the limitation of dorsiflexion of the 1st MTP joint and seeing, and accommodating to, the demands of the need for more dorsiflexion at toe off.
But, here is the kicker. You have likely seen this video of ours on Youtube on how to acquire a foot tripod from using the toe extensors to raise the arch. Video link here and here. Well, in his patient’s case today, they have a limitation of 1st MTP dorsiflexion, so the ability to maximally raise the arch is impaired. The Windlass mechanism is broken; “winding” of the plantar fascia around the !st MTP mechanism is not sufficiently present. Any limitations in toe extension (ie dorsiflexion) or ankle dorsiflexion will mean that :
1. compensations will need to occur
2. The Windlass mechanism is insufficient
3. gait is impaired at distal swing phase and toe off phases
4. the anterior compartment competence will drop (Skill, endurance, strength) and thus injury can be more easily brought to the table.
In this patient’s case, they came in complaining of burning at the top of the foot and stiffness in the anterior ankle mortise area. This would only come on after a long brisk walk. If the walk was brisk yet short, no problems. If the walk was long and slow, no problems. They clearly had an endurance problem and an endurance challenge in the office showed an immediate failure in under 30 seconds (we will try to shoot a quick video so show our little assessment so be patient with us). The point here today is that if there is a joint limitation, there will be a limitation in skill, strength or endurance and very likely a combination of the 3. If you cannot get to a range, then any skill, endurance or strength beyond that limitation will be lost and require a compensation pattern to occur. This patient’s arch cannot be restored via the methods we describe here on our blog and it cannot be restored by an orthotic. The orthotic will likely further change, likely in a negative manner, the already limited function of the 1st MPJ. In other words, if you raise the arch, you will shorten the plantar fascia and draw the 1st MET head towards the heel (part of the function of the Windlass mechanism) and by doing this you will plantarflex the big toe … . but weren’t we praying for an increase in dorsiflexion of the limitus big toe ? ……..yes, exactly ! So use your head (and spank the orthotic when you see it used in this manner. ”Bad orthotic, bad orthotic !”)
So think of all of this the next time you see a turf toe / hallux rigidus/ hallux limitus. Rattles your brain huh !?
This is not stuff for the feint of heart. You gotta know your biomechanics.
Shawn and Ivo … .the gait guys
Addendum for clarity:
a Facebook reader asked a question:
From your post: “if you raise the arch, you will shorten the plantar fascia and draw the 1st MET head towards the heel (part of the function of the Windlass mechanism) and by doing this you will plantarflex the big toe … . but weren’t we praying for an increase in dorsiflexion of the limitus big toe ? ” I always thought when the plantar fascia is shortened, it plantar flexes the 1st metatarsal (1st ray) and extends (dorsiflexes) the 1st MTP joint….
Our response:
We should have been more clear, our apologies dear reader. Here is what we should have said , ” The plantar fascia is non-contractile, so it does not shorten. We meant conceptually shorten. When in late stance phase, particularly at toe off when the heel has raised and forefoot loading is occurring, the Windlass mechanism around the 1st MET head (as the hallux is dorsiflexing) is drawing the foot into supination and thus the heel towards the forefoot (ie passive arch lift). This action is driving the 1st MET into plantarflexion in the NORMAL foot. This will NORMALLy help with increasing hallux dorsiflexion. In this case above, there is a rigid 1st MTP joint. So this mechanism cannot occur at all. In this case the plantar fascia will over time retract to the only length it does experience. So, if an orthotic is used, it will press up into the fascia and also plantarflex the 1st MET, which will carry the rigid toe into plantar flexion with it, IN THIS CASE.”