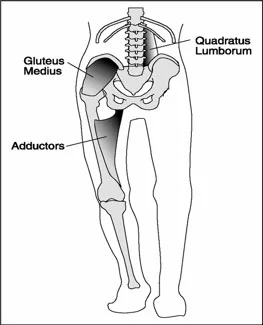
Sometimes you may need to put the cart before the horse...The knees, the glutes and reverse engineering ?
/We have talked about looking at things “from the bottom” up in the past, so we can understand things like why the vastus medialis is an external rotator in closed chain as are the semi membranosis and tendinosis. Perhaps we need to think more about this traveling proximally, where the knee effects the glutes. We found this paper looking at women with patello femoral problems and gluteal inhibition. Prospective studies have not found gluteal weakness to be a risk factor for patello femoral problems, but perhaps it is the other way around and patello femoral problems are a risk factor for gluteal weakness? It makes sense, especially if you consider the vastus lateralis like we talk about here and here.
“We hypothesize that muscle inhibition is present in the gluteal muscles of females with PFP compared to healthy controls and it is associated with both decreased subjective function and longer duration of symptoms.”
Dr Ivo Waerlop, one of The Gait Guys
Glaviano NR, Bazett-Jones DM, Norte G. Gluteal muscle inhibition: Consequences of patellofemoral pain? Med Hypotheses. 2019 May;126:9-14. doi: 10.1016/j.mehy.2019.02.046. Epub 2019 Feb 27.
#gait #foot #patellofemoralpain #PFP #quadriceps #thegaitguys #glutes #gluteal muscles